© 2016 Sarkar AMITABHA
2016 – №2 (12)
 Abstract: Mortality due to hunger is historically a common public health event and pertinent even in current context. The modern approach of public health views it under the narrow bio-medical thinking ignoring the entire social realities. Social epidemiology as a public health tool has enormous potency in defining such public health phenomenon using historical trends, contextual factors and human body conditions.
Abstract: Mortality due to hunger is historically a common public health event and pertinent even in current context. The modern approach of public health views it under the narrow bio-medical thinking ignoring the entire social realities. Social epidemiology as a public health tool has enormous potency in defining such public health phenomenon using historical trends, contextual factors and human body conditions.
The paper develops a ‘Hunger-Mortality’ skeletal diagram to depict how hunger as a root cause gets formed because of unavailability of food and accordingly the human body is being affected and succumbed to death or disease. Mortality appears under the simplified but non-negotiable ‘hunger chain’: food unavailability – undernutrition – compromised immune system – susceptibility to infections – higher risk of morbidity/mortality.
The paper further takes the reference of study conducted by Sheila Zurbrigg in the context of Punjab, India to explain causes of malaria mortality in colonial India during 1868–1940. This study delineates the thinking of social epidemiology to trace the causality of malaria mortality.
The paper uses the perspective of social epidemiology to explain the importance of food in relation to hunger and mortality and critical to the popular practice of micronutrient level intervention to address hunger.
Keywords: Social Epidemiology, Hunger, Mortality, Food, Nutrition, Micronutrient
‘There are people in the world so hungry, that God can not appear to them except in the form of bread.’ This famous quote of Mahatma Gandhi ironically and accurately represents the grimness of hunger and its sin to the human population. Hunger is caused by many grave issues and similarly it leads to many complex consequences. Both the causes and consequences are predominantly interlinked to the socio-politico-economic gravity of understanding. The most common and severe result of hunger is mortality. The science of medicine defines mortality as the outcome of diseases occurred from any parasitic invasion or persisting risk, and thus underrate the role of basic determinants of health. This view gets recognised and referred most of the time to maintain the harmony of ‘power equation’ which includes various state actors, from industrial lobbies to political pressure groups. However, this power equation is unable to clarify the concerns of real public health outlook. The relation between hunger and mortality is a ’cause and effect equation’.
The philosophy of public health has well defined framework to explore such ‘equation’ but, alas, over-dependency on bio-medical science has been for long instrumental ignoring the known and effective practice of bio-social understanding. The transformation of epidemiology as a public health tool has narrowed down both the idea and practice of finding ‘causality’ from population level to cell/molecule level. Thus, the epidemiological exercise has become more positivist rather than realist and context-free instead of historical and cultural analysis (Pearce 1996). This piece of writing takes the perspective of social epidemiology to understand and analyze a common public health event that is mortality due to hunger. This writing does not offer nuances of social epidemiology paradigm. Rather, it analyzes the causality between hunger and mortality using social epidemiology perspective and then furthers the discussion by taking reference of one case study from Punjab province in India.
Understanding causality between hunger and mortality can be well addressed under the framework of hunger – food – nutrition – immunity – infection probability – mortality. Hunger (the root cause) has detrimental effects and those effects cumulatively but in tandem cause mortality (the outcome effect). The cause of hunger is rooted in the basic modalities of production and distribution of resources where skewed production of food and/or unequal distribution of basic needs and wants brings about hunger in the population. Hunger has two types: acute (starvation) and chronic (undernutrition). Both types of hunger occur mostly in three possible forms: food shortage, food poverty and food deprivation (Messer et. al. 1997). These forms of hunger can happen to any population or an individual separately or in sequence. Food shortage occurs when the market experiences unexpectedly decline in food production, which disturbs the chain of availability of food among the defined population and provokes extremely high prices (lack of accessibility because of food poverty), finally resulting in sever nutritional deficiency for that population because of inadequate food intake (food deprivation). These food factors are socially determined, politically contextualised and economically dependent, and can’t be explained by solely individual reasons.
The second factor is nutrition, the component in human biological system which is determined by the food consumption characteristics. Nutrition is required for physiological activity and healthy life. Lack of food means lack of nutritional input to the body that manifests in forms of malnutrition and micronutrient insufficiency. Malnutrition, popularly known as Protein-Energy Malnutrition (PEM), is the most often clinically observed condition among the hunger-affected people. It leads to energy deficiency, weight loss and even marasmus (clinically diagnosed severe form of malnutrition). Food scarcity also leads to micronutrient insufficiency among the population. Iron, iodine and vitamin A are the most common micronutrients which any individual gets deprived of during the period of hunger. Iron deficiency causes anemia, especially among women and children. In the long run, anemia creates problems for physical activity and development of cognitive processes. The shortage of second important micronutrient, iodine, provokes mental disability; in the long run symptoms of a goiter are also found. Insufficient Vitamin A results in blindness and many other complications. There are other less known micronutrients which have vital role in protecting human health from various diseases. Niacin against pellagra, thiamine against beriberi; vitamin C against scurvy; vitamin D against rickets are few of such examples. The whole nutritional status becomes endangered when one gets deprived of food; this situation eventually leads to many diseases (Messer et. al. 1997).
Understanding the relationship between nutrition and infection started to be formulated at the end of the Second World War. In 1965 WHO (World Health Organization) conducted a meeting of experts to examine the interrelationship of nutrition and infection, and by 1968 a monograph was published entitled ‘Interactions of Nutrition and Infection’ (Scrimshaw, Taylor and Gordon, 1968). The monograph was based on the past evidence of epidemiological, clinical and experimental exercises (Shetty 2010). The causal chain of hunger continues from food to nutrition to infection, but the immunity status also plays an important role for development of infection from the stage of undernutrition. The immunity system goes down at the time of starvation or in the state of undernutrition. Undernutrition leads to ‘nutritional immunodeficiency’, when the body loses its immunity faster and becomes vulnerable to any infectious agents (or microorganisms) (Shetty 2010). The infection can not appear all of a sudden, it depends on the relation between the host (human body) and the agent (microorganism). This relation is balanced by the immune system. The infection occurs when this balance gets broken. The immune system protects the body from invading microorganisms but, because of compromised nutritional status, the same immune system gets weakened, leaving the human host at greater risk of infection. The role of immune system, compare to food and nutrition, is often neglected in the relationship between hunger and mortality; still, the medical science itself confirms that without the compromised phase of immune system the infectious agent can not get multiplied inside the body of human host.
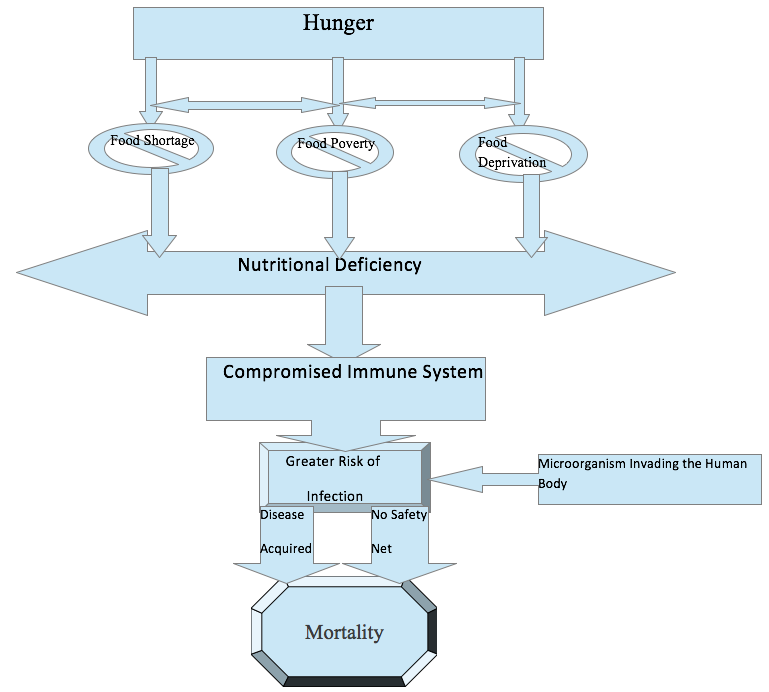
The below ‘Hunger-Mortality’ skeletal diagram explains how hunger (as a product of societal cause) causes mortality at individual or population level.
The ‘Hunger-Mortality’ skeletal diagram:
The outcome effect of hunger is mortality. Mortality appears under the simplified but non-negotiable ‘hunger chain’: food unavailability – undernutrition – compromised immune system – susceptibility to infections – higher risk of morbidity/mortality. An individual develops diseases while in hunger; he/she becomes more prone to death as hunger multiplies with poverty, inequality and lack of access to needed provisions. The above diagram is a logical exercise based on the relationship ‘nutrition – immune system – infection’ at an individual level or within human body system, but that is only a half of causality. A lack of nutrition is non-availability of food which has its own political economy context. The scope of social epidemiology is capable to relate this political economy context with morbidity/mortality in society or in individual. The political economy may appear in the form of food shortage/ food poverty/ food deprivation. The social epidemiological perspective can identify the particular form of food crisis and reasons behind that and accordingly plan effective measures.
The present and past events of hunger may be similar or different from each other depending on the context. The debates address the questions of whether the past events of hunger were natural or man-made or even whether they happened at all. Similarly, the human toll resulted from those events are till date controversial because of the political nature of inquiry and epidemiological scope of scrutiny. The association between hunger and mortality is further reviewed in reference to the paper written by Sheila Zurbrigg on mortality caused by malaria in Punjab (‘Re-Thinking Public Health: Food, Hunger and Mortality Decline in South Asian History’ (Zurbrigg 2001)). The study of epidemic history had been conducted in Punjab, India in pre-independence era. The study period was from 1868 to 1940. It dealt with the causes of a series of mortality episodes during the specified era. Like any other historical epidemiological investigation, it had also faced inconspicuous data and biased documentation referring to politically tailored information. The study was an honest effort to examine the series of events and rethink a larger picture of public health via social epidemiology perspective covering macroscopic issues (those beyond the agent-microorganism relations theory).
The author, Sheila Zurbrigg, started with the idea that the approach to studying public health problems had changed. The disease-specific intervention (curbing the spread of microorganisms through hygiene and improved sanitation) which made part of the public health approach had come after the landmark sanitary movement in England lead by Edwin Chadwick in the second half of the nineteenth century. This line of the approach was continuously modified over the centuries in accordance with technological development (medication, controlling of disease agents). The pre-Chadwickian era mostly took into consideration the basic economical and social factors behind the human suffering. The shift in thought and approach made the public health more complex and technically dependent over the years. This change in thought, approach and finally in practice are characterized by the trace of complex political vendetta and market modalities. That was the argument in the study presented under the analytical framework of mortality investigation. It challenged the notion of technology-driven modern medical science considered to be the key factor in decreasing mortality and increasing life expectancy. The study referenced Thomas Mckeown’s work (1976) to give support to significance of basic determinants of health behind the gradual rise of life expectancy in various parts of the world. Mckeown et. al. (1976) thesis was complemented by contemporary historic anthropometric analysis conducted in a number of European populations where the improved nutrition status was found to be strongly effective in mortality decline. Indeed, Zurbrigg’s study provided critique on research works which ended up specifying hunger as ‘unscientific, imprecise and even emotional’ conclusion in reference to any large-scale mortality reasons. The study pointed out that the hunger effect got neglected also because of the mystified differentiation between acute and chronic hunger.
The study brought up the peculiar South Asian health history in order to explain the case of malaria mortality decline in Punjab. Modern medicine was ascribed the leading position in this issue. The DDT (Dichloro Diphenyl Trichloroethane) intervention under malaria control programme was considered the supreme factor in bringing down the death rate. The role of hunger was hardly scrutinized with much detail, thus famine or flood control, curb on resource exploitation, and the relief activities were administered in a piecemeal approach without any operational strategy. The author’s past observational experience in rural Tamil Nadu, India, related to provision of basic healthcare services and DDT to help decrease mortality from malaria made the author cautious about buying the logic of technological justification for mortality decline. Interestingly, the death rate started to decline from 1911 onwards (Zurbrigg’s paper; figure-10.4), but the DDT came into effect widely in India from 1953 onwards, under the National Malaria Control Programme (1953). Punjab region was chosen by the study because malaria was a major cause of death here before 1920, which was supported by the evidence of fever death records captured in colonial sanitary reports (one of the few places in South Asia). Fever death was the only available tool to track malarial mortality during 1868 to 1948 because of ungrouped data under fever disease. However, the study accepted the justification of epidemiological and entomological behavior which suggested that malaria transmission (specifically the falciparum infection) usually occurred in the late monsoon and the immediate months after it. The study considered fever death rates of that season only for the investigation purpose.
The study presented epidemiological, entomological and environmental instances to prove the relation between malaria mortality and socio-economic factors. It recognized that the autumn season faced a sharp rise in malarial deaths and the infection (in particular the falciparum infection) was not quite chronic during the month of monsoon. This finding can be proven by looking at the clinical progression of the infection: malaria infection takes fourteen days on average to manifest, so, if the monsoon session is considered as a breeding period, post-monsoon is the period when the infection gets matured and manifests its symptoms. Hence, the study mentioned these events by adducing epidemiological and entomological explanation. The study showed that the mortality from malaria fluctuated in a sawtooth fashion from 1868 to 1908 (Zurbrigg’s paper; figure-10.5). The malarial death rates were significantly lower from 1908 onwards compared to those in 1868–1907, despite there was hardly any noticeable change in the incidence of rainfall or flood in Punjab that could influence the mosquito breeding for the entire study period (1868 – 1940). The change occurred not only in the number of malaria infection before and after 1908, but also in malarial mortality rate which declined after 1908. The newly developed medical treatment could not be the cause for decrease in malaria death rates, as per capita availability of quinine was very low, especially in rural areas up until late 1930s. This meant that the needed dose of quinine was much smaller than the one actually required for an effective intervention. So, both the rainfall-flood and medical intervention factors did not hold any merit. The only factor which changed after 1908 was famine. The period from 1868 to 1908 saw great malaria epidemics and also faced the incidence of ‘frank famine’ (officially recognized by the colonial Govt.) or sudden economic vacuum because of large-scale grain exports. (One exception was 1876’s epidemic which took place on the backdrop of a devastating flood which took place in 1875.) The effect of famine or large-scale grain exports needs to be seen as economic consequences (excessive price hike of food grains) to the population. The author confirmed the correlation between malaria mortality and food grain price hikes for the period from 1868 to 1908 through multiple regression analysis. The study further cited that 22 out of 24 districts in the then Punjab province showed significant relationship between malaria mortality and food grain price hike.
In the second part, the study dealt with the measures initiated to bring down the malaria mortality. Malaria control activities were conducted locally in urban slums. Few policy-level changes were made, like setting up of ‘famine code’ (official recognition of famine by the government based on certain conditions, such as severe harvest failure) in 1883 and drought relief activities from 1908 onwards. The study cautiously noted that the short-term relief could not address the chronic hunger cases (undernourishment). The medical interventions, quinine support and DDT provision were already shown to contribute nothing or little to bringing down the mortality rates during the studied period. Evaluation of DDT meaning for malaria mortality decline was never measured because of inconspicuous data. Though it is always acknowledged that DDT use was initially very much effective in controlling the malaria infection, the point that this study made was that the life expectancy started to increase or crude death rates started to decrease much earlier that the massive use of DDT (Zurbrigg’s paper; figure-10.1 and 10.6 for Ludhiana district as a case example). This set of information revealed that the govt. initiative in the form of situation-based support (relief activities) or technological measures could not encompass the actual reasons behind the mortality decline from malaria infection.
The author singled out four types of relationships to describe the role of socio-economic factors in mortality decline. The study period was 1868-1940, and the relationships also relate to this time interval.
Relationship I: The statistical significance of correlation between malaria mortality and rainfall remained the same even after 1908 when the rate of mortality from malaria epidemics steadily declined. So, the rainfall could be related to the spread of malaria, but there were other factors which influenced malaria mortality rate.
Relationship II: The multiple regression statistically showed that the relation between malaria mortality and food grain price levels became irrelevant after 1908. Indicatively, the relief activities became a common intervention measure from 1908 onwards and expanded this solidarity in subsequent years.
Relationship III: The historical records of colonial govt. before 1910 alluded to the close link between the famine, economic crisis (due to agricultural imbalance), food scarcity and malaria mortality. This information fact could be further traced in the annual reports made by ‘provincial sanitary commissioners’ during the nineteenth and early twentieth century. Those reports included pointers of prices for staple food, wage rates and state of the harvests which allows to outline the economic conditions of the that locality. Similarly, those reports also gathered facts on larger malarial deaths among starving populations during the period of study. Hence, these two separately collected sets of data for preparing those annual reports currently can be contemplated for the historical epidemic investigation purpose. The integrative mode of analysis suggests to relate the famine to economic scarcity followed by food grain crisis which resulted in malarial deaths.
Relationship IV: The relation between nutritional status and malaria is the cardinal point of consideration which the study made in order to explain the historical evidence under modern medical theory. The author argued that the malaria-nutrition relationship has been considered as less important in modern medical texts, because they focus only on the micronutrient deficiencies and to some extent on the issue of malnutrition (chronic hunger). The acute hunger (starvation) under the context of nutritional value has never been a considerable point of analysis; thus, the concept of acute hunger was lost. So, the author claimed that the modern nutrition science could not relate the acute hunger (often caused by famine or flood during 1868 – 1908) with malaria mortality.
The author framed the malaria problem as a nutritional issue and encouraged public health reflection on nutritional factors that could also be included into its approach to hunger. The author acknowledged that malaria deaths were undoubtedly low during the 1950s because of DDT intervention. Using the same principle, it could also be deciphered that the same malaria mortality was much higher much before the DDT intervention (before 1908), while the malaria infection was factored by epidemic starvation. In the concluding part of the study, the author referenced a few other instances from different countries to support the relation of mortality with nutritional access through food. In a similar manner, an international hike in food grain prices during 1973-74 and troublesome national food subsidy programme in Sri Lanka led to higher rates of child mortality in 1974.
The study questioned the technological determinism in answering the basic public health problem. The technological advancement is in line with Cartesian understanding of the body (the body is a machine and treatment of diseases is similar to re-fixing machine parts) which made health issues more complicated and market-based. Disease is not only about chemical imbalance inside the body or invasion of any microorganism, but certainly the origin of its history or cause. Quinine may cure the malaria infection, DDT may effectively control the microorganism by destroying its source, but what happens if quinine is not available or accessible to all the needy people or if microorganisms develop resistance to DDT?
These thoughts give birth to the central question pondered by the author: ‘what causes malaria?’ and not ‘why malaria?’. The basic inequality exists across class, caste and gender which has many health outcomes, be it in nineteenth century or twenty first century. Hunger is one of the many products of inequality which cannot be resolved by a technological solution. It was the exploitative nature of the colonial rule and social stratification which made the poor class more susceptible to malaria. By addressing the relation between hunger and malarial mortality, the author asks the question why the hunger occurs and who mostly gets affected. In other words, it was the nutrition (or food) purchase capacity of the people which became the risk factor of malaria mortality during the acute food crisis. The author lists the reasons for food shortage-food poverty-food deprivation conditions after analyzing the cause of the events occurred during that phase and also observes that inequality determines the strata in the society and vulnerability. During the British regime, it was the shift from staple crop to cash crop which created acute food shortage. Food shortage was also influenced by the practice of food export during the British regime which resulted in acute food scarcity inside the country. In both cases, because of food shortages the poor people suffered most, since they were unable to purchase the basic means of life. Besides, in the nineteenth century the policy of cheap cotton garments imported from England made many Indian workers related to cotton industry jobless and pushed towards poverty. Further, the events of food crisis (followed by acute hunger) were aggravated for the artisan class by the practice of food holding by the big farmers. It was the colonial regime whose continuous practice of resource drainage from India to Britain made the marginalised or lower class people more vulnerable in terms of accessing food, being easily infected with malaria and succumbing to death. The author further contextualised the malaria mortality in debates around food security and asserted that the poor ‘cannot hope to buy their way out of the failure of basic public services through bottled mineral water’; rather the discussion must ‘shift to food security in explaining mortality decline in India’.
The earlier sketched ‘Hunger-Mortality’ diagram has rated the ‘safety net’ a precondition for mortality once the human being acquired disease. This safety net is all about the socio-economic protection which may save individuals from the sin of disease. Surely this socio-economic protection does not exist across the class-caste-gender, thus the gap of disparity gets widened. Zurbrigg’s work is the classic explanation of the malarial mortality decline, which is not limited to the science of nutrition only, but is also rooted in the scream of socio-economic inequality. The current practice of so called modern epidemiology may relate it to the micronutrient deficiency or molecular imbalance. However, the holistic perspective of social epidemiology takes the trouble to not only explain the source of disease but also the cause of disease.
References
Mckeown T., Brown R.G., Record R.G. (1976) An Interpretation of the Modern Rise of Population in Europe, Population Studies, Vol. 26, No.3, p. 345-382.
Messer E., DeRose L., Millman S. (eds.) (1997) Who’s Hungry? And How Do We Know? Food Shortage, Poverty, and Deprivation, United Nations University Press.
Pearce N. (1996) Traditional Epidemiology, Modern Epidemiology, and Public Health, American Journal of Public Health, Vol. 86, No.5, p. 678-683.
Shetty P. (2010) Nutrition, immunity, and infection, Cambridge University Press.
Zurbrigg S. (2001) Re-Thinking Public Health: Food, Hunger and Mortality Decline in South Asian History. Qadeer I., Sen K. and Nayar K. (eds.), Public Health and Poverty of Reforms: The South Asian Predicament, Sage Publications. New Delhi, p. 174-197.